Seeking substance use disorder treatment shouldn’t mean sacrificing your privacy. At EveningIOP, we understand that confidentiality is essential to your recovery-it protects your job, your relationships, and your dignity.
Privacy-focused SUD care isn’t a luxury. It’s a practical foundation that lets you focus on healing without fear of judgment or exposure.
How Your Privacy Gets Protected
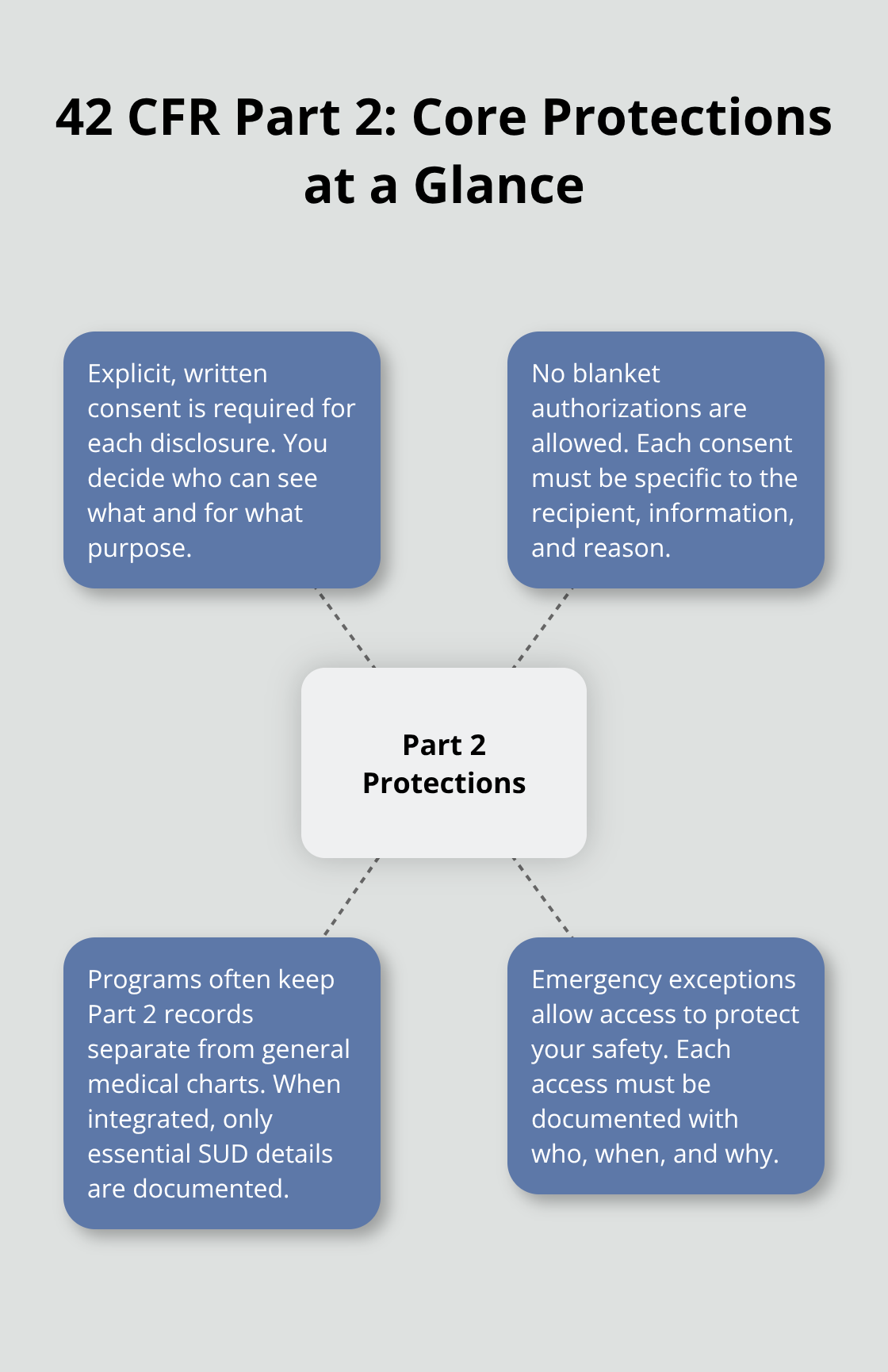
Federal law treats substance use disorder records differently than other medical information, and this distinction matters enormously for your safety. Under 42 CFR Part 2 substance use disorder confidentiality rules, any program that receives federal funding to treat substance use disorders must follow stricter confidentiality rules than standard HIPAA requires. This means your treatment records cannot be shared with employers, insurers, or family members without your explicit written consent for each disclosure. The law prohibits blanket authorizations, so you control exactly who sees what. When you sign consent forms, they must specify the recipient by name or title, the information being shared, and the purpose. This level of specificity prevents unauthorized access and limits exposure.
Separate Records Protect Your Information
Many treatment programs maintain Part 2-protected records completely separate from general medical records, which adds another layer of protection. If you receive care in a facility that integrates substance use treatment with other medical services, clinicians document only essential SUD information in your general medical chart to minimize unnecessary exposure. Emergency exceptions exist-if you face an immediate health threat, medical personnel can access your records without consent, but the program must document who accessed the information, when, and why.
Coordination of Care Requires Your Consent
Coordination of care is essential for safety, especially when you take medications like buprenorphine or naltrexone, since harmful drug interactions can occur. When your SUD program needs to share information with your primary care doctor or emergency department, they must obtain your written consent first. You can revoke this consent at any time, and revocation applies only to future disclosures-past ones remain valid. If a third-party organization like a health information exchange wants to handle your records, your treatment program signs a Qualified Service Organization Agreement that legally binds them to maintain confidentiality. Electronic systems add complexity because Part 2 rules still apply to data moving through health information exchanges, and SAMHSA provides specific guidance on this. Ask your treatment provider to explain their data-sharing agreements before you sign anything. Know whether your records go into a shared system and who has access.
Technical Safeguards Keep Your Data Secure
Secure messaging, encrypted files, and restricted access logs form the technical backbone of privacy protection. Treatment platforms use end-to-end encryption for telehealth sessions and secure storage for your records, meaning only authorized clinicians can view your information. When programs use fax, phone, or electronic transfers, risks increase-data can be misrouted or intercepted. Modern programs minimize these risks through automated systems and strict training on proper handling. Ask your provider whether they use secure patient portals with audit logs showing who accessed your records and when.
State Laws Add Extra Protections
Many states add extra protections: Maryland, New Jersey, and the District of Columbia restrict what can be disclosed beyond federal requirements. If you move between states or use out-of-state providers, state laws matter. Your treatment program should know these rules and apply the stricter standard in your situation. Understanding these protections helps you make informed choices about where you seek care and what information you authorize for sharing.
Why Privacy Matters for Your Recovery
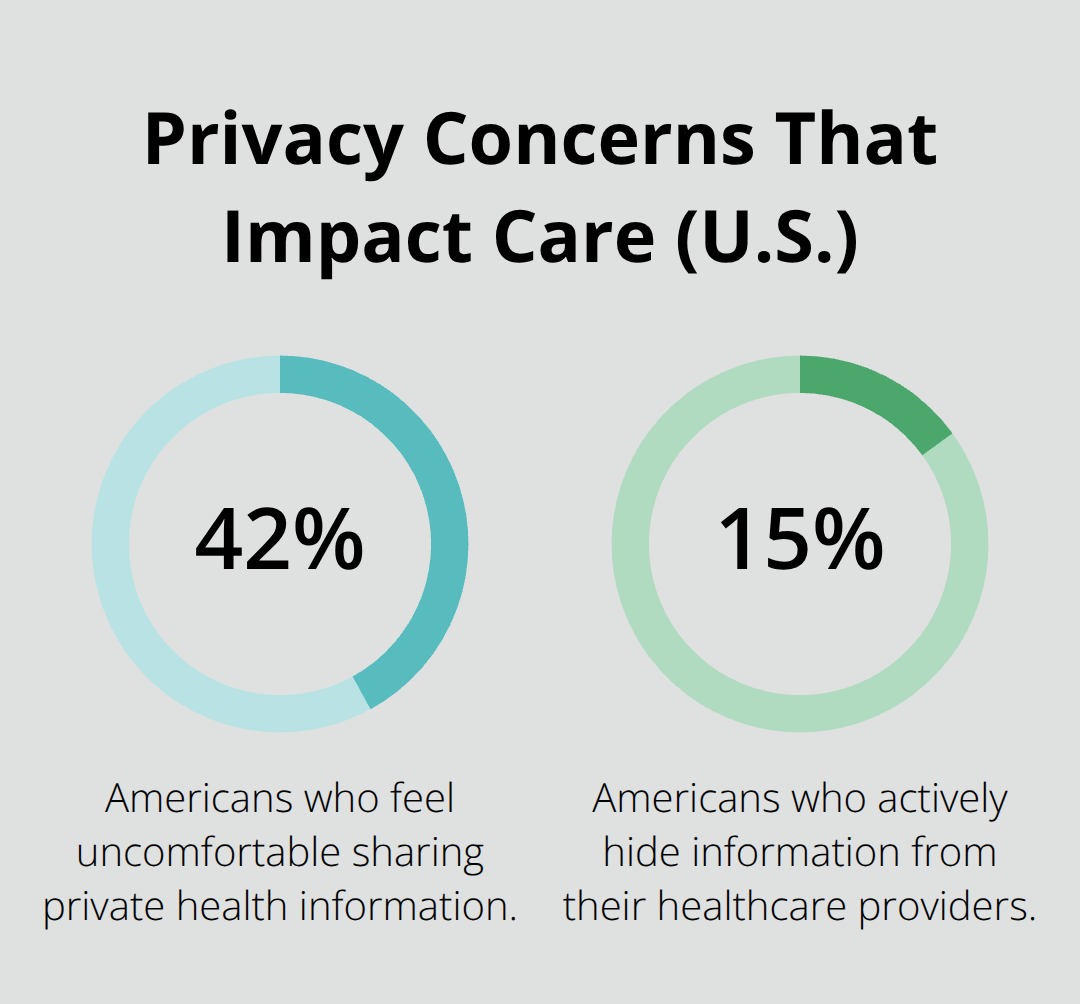
Privacy in substance use disorder treatment isn’t abstract-it directly affects whether you’ll seek care, stay engaged, and build a life free from fear. About 42% of Americans feel uncomfortable sharing private health information, and 15% actively hide information from their healthcare providers, according to a national consumer survey. That hesitation costs lives. When people fear exposure, they delay treatment, skip appointments, or avoid disclosing co-occurring mental health conditions that require integrated care. Confidentiality removes that barrier.
How Privacy Shapes Your Honesty in Treatment
Federal protections under 42 CFR Part 2 exist because research shows patients disclose more honestly and engage more fully in recovery when they know their records stay private. This matters practically: honest disclosure helps your clinician catch dangerous drug interactions, identify trauma that drives substance use, and adjust medications like buprenorphine based on your actual experience rather than guesses. Without privacy protections, you manage recovery with incomplete information. Licensed clinicians understand that confidentiality is foundational to effective care-without it, patients withhold information about relapse, medication side effects, or behaviors that feel shameful.
Employment and Family Remain Protected
Employment protection is concrete and urgent. Employers cannot legally access your substance use treatment records under Part 2, even if they’re paying for your insurance. This distinction separates SUD records from general medical records deliberately-your boss will never see that you’re in treatment unless you tell them. Family members also cannot access your records without your written consent. This matters when family dynamics complicate recovery or when past trauma involves people in your household.
You control who knows what, and you can revoke access at any time.
Building Trust Through Transparency
Trust with your treatment team requires transparency about data handling, not just clinical skill. Your provider should explain their specific data-sharing practices before you sign consent forms. Ask whether they use secure messaging, how long records are stored, and what happens if you move to another state. Request a written confidentiality policy. Programs that integrate substance use treatment with mental health care or primary medicine must document only essential information in shared records to minimize exposure.
One practical step: ask your treatment provider whether they maintain separate Part 2 records or integrate SUD information into a general chart. If information goes into a shared health system, confirm who has access and request an audit log showing what’s been viewed. If your provider resists these questions or dismisses confidentiality concerns, that’s a red flag about their commitment to your safety. Strong clinical programs welcome these conversations because they know privacy builds the trust necessary for honest, effective treatment.

Your recovery depends on feeling safe enough to be fully yourself with your clinician-and that safety starts with understanding exactly how your information moves through the healthcare system.
Privacy-Protected Care That Fits Your Schedule
Telehealth has transformed substance use disorder treatment from a rigid daytime commitment into something that actually works with real life. Telehealth adoption for addiction treatment rose approximately 70% between 2020 and 2023 according to Centers for Medicare and Medicaid Services data, and that shift happened because virtual care solves a fundamental problem: people with jobs, families, and responsibilities can now access treatment without broadcasting it to their employer or coworkers.
How Secure Telehealth Protects Your Information
Encrypted video sessions, HIPAA-compliant data storage, and audit logs form the technical foundation of privacy-focused virtual care. These systems show exactly who accessed your records and when. When you choose a telehealth program, ask whether sessions use end-to-end encryption and whether the platform stores your video recordings. Many programs claim security but store unencrypted files or keep indefinite session logs. Legitimate programs delete session recordings after a defined period and limit access to licensed clinicians directly involved in your care. Insurance coverage has expanded significantly-the Centers for Medicare and Medicaid Services now reimburse virtual addiction treatment, peer support, and medication-assisted treatment at parity with in-person care, meaning your out-of-pocket costs remain identical whether you attend in person or online. This parity reflects evidence that virtual care produces outcomes matching in-person treatment. When you enroll in a telehealth program, request their privacy policy in writing before your first session and confirm they maintain separate Part 2-protected records rather than mixing SUD information into a general medical chart.
Anonymous Support Communities Online
Peer support groups online serve a different function than clinical treatment-they provide connection without clinical assessment or medication management, which appeals to people who prioritize anonymity over professional oversight. Platforms like SMART Recovery and AA meetings conducted through Zoom offer genuine community, but understand the privacy distinction: peer support groups typically operate outside Part 2 protections unless they’re formally affiliated with a federally assisted program. This means the group operator isn’t legally bound to maintain confidentiality the way a treatment provider is. If anonymity matters most to you, choose groups that explicitly don’t collect identifying information and use pseudonyms throughout.
Remote Drug Testing Keeps Results Private
Remote drug testing integrated into clinical programs adds practical privacy: instead of traveling to a lab or clinic for observed testing, you complete tests at home using a kit mailed to you or collected from a secure drop box. The results go directly to your clinician through the same encrypted system as your therapy notes, not to your employer or insurance company unless you authorize it. This matters because traditional lab-based testing creates a paper trail-your employer’s occupational health department may see test results, or insurance systems may flag positive screens. Home-based testing keeps that information contained within your treatment relationship. When selecting a program, confirm whether remote testing results are automatically reported to third parties or whether results go only to your treatment team by default. Some programs require explicit authorization before sharing any testing information, which gives you control over who learns about your test results. The strongest privacy-focused programs treat remote testing as part of clinical documentation under Part 2 protections, not as a separate reporting system to employers or payers. Evening group therapy options further expand access by removing scheduling barriers while maintaining confidentiality.
Final Thoughts
Privacy-focused SUD care works because it removes the fear that prevents people from seeking help. When you know your treatment records stay protected, you can be honest with your clinician about relapse, medication side effects, and the struggles driving your substance use. That honesty changes everything-it lets your treatment team catch dangerous drug interactions, identify trauma, and adjust your care based on what’s actually happening in your life.
Taking control of your treatment experience means asking direct questions before you enroll. Ask whether your program maintains separate Part 2-protected records or mixes SUD information into a general medical chart, request their written confidentiality policy, and confirm who has access to your information. Strong programs welcome these conversations because they understand that privacy builds the trust necessary for honest, effective recovery.
Your next step is finding a program that matches your life and your privacy needs. EveningIOP offers live telehealth evening Intensive Outpatient Programs that combine interactive group therapy, one-on-one sessions with licensed clinicians, and remote drug testing-all designed so you can pursue recovery without disrupting work or family responsibilities. The program is DHCS-licensed, Joint Commission-accredited, and LegitScript-certified, meaning clinical quality and privacy safeguards are built in from the start.


