Addiction treatment shouldn’t force you to choose between recovery and your career. At EveningIOP, we’ve built a program specifically for working professionals who need flexibility without compromise.
Evening IOP accessibility means getting the clinical care you need on your schedule, not ours. That’s how real recovery happens for busy people.
Why Evening Programs Matter for Working Professionals
The Cost of Choosing Between Work and Recovery
Traditional daytime treatment programs force working people into an impossible choice. A standard Intensive Outpatient Program typically requires 9–15 hours of therapy per week during business hours, which means taking time off work, risking your job stability, or lying to your employer about where you are. For someone earning $50,000 annually, missing even two weeks of work costs roughly $1,923 in lost income. That financial pressure alone keeps many people from seeking help.

Evening IOP removes this barrier entirely. Treatment happens after 5 p.m., so you clock out from work, attend your sessions, and maintain your paycheck and professional reputation. This isn’t a compromise on care quality-it’s simply clinical treatment delivered at a time that actually fits your life. The data backs this approach: according to program outcome reports from providers using this model, participants can maintain employment while receiving treatment. That’s not incidental-that’s transformative for someone’s long-term recovery and financial stability.
How Evening Programs Solve the Childcare Problem
Evening flexibility solves the childcare crisis that stops parents cold. A single parent with two kids cannot simply disappear for three hours five days a week during daytime programming without paying for emergency childcare or pulling children from school. Evening programs let parents handle their parenting responsibilities first, then attend treatment when kids are home or in the care of a partner.
The same logic applies to caregivers supporting aging parents, students managing course schedules, and people without reliable transportation. Remote telehealth components eliminate commute time entirely-no sitting in traffic, no missed sessions because the bus ran late. This accessibility matters because treatment completion rates depend heavily on people actually showing up. When your program fits your life instead of forcing your life to stop, you attend consistently, engage more deeply, and build real recovery momentum.
What Happens When Treatment Actually Fits Your Schedule
Live telehealth group therapy sessions, one-on-one meetings with licensed clinicians, and remote drug and alcohol testing all happen in the evening hours when you’re available. You participate from home, eliminating barriers that derail people from traditional programs. The structure remains rigorous-you still receive the same clinical intensity and accountability-but the timing removes the friction that prevents people from starting treatment in the first place.
This model works because it acknowledges a simple truth: recovery happens when people actually show up. Evening IOP removes the biggest obstacle to treatment access, and that changes everything about whether someone can sustain their commitment to recovery.
The Structure Behind Evening Treatment
How Group Therapy Anchors Evening Programs
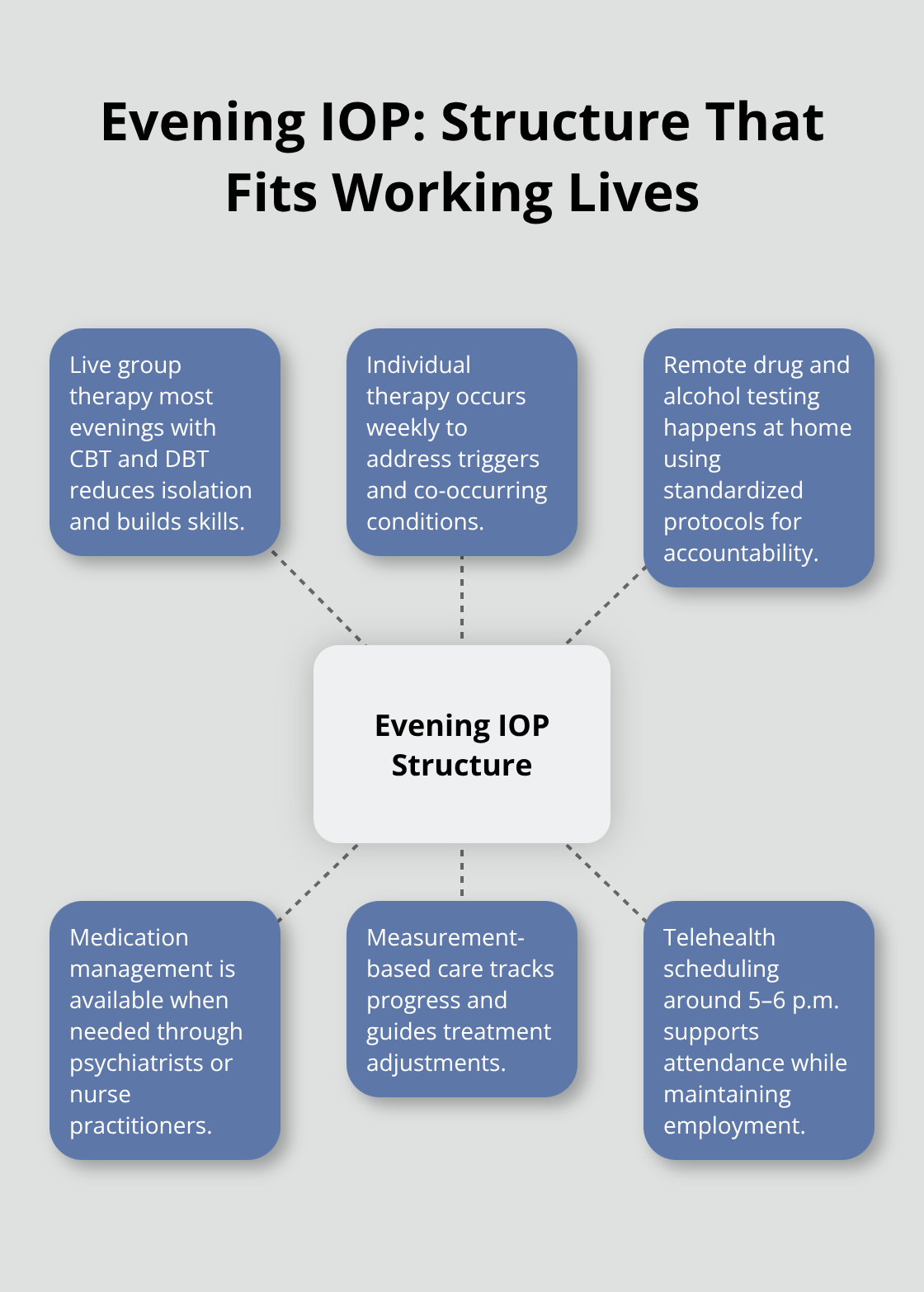
Evening IOP operates on a principle that clinical intensity and daytime flexibility work together. Live telehealth group therapy sessions form the backbone of treatment, happening most evenings where participants connect with peers facing similar challenges and engage in evidence-based modalities like Cognitive Behavioral Therapy and Dialectical Behavior Therapy. These sessions typically run 60 to 90 minutes, and the group format matters because isolation fuels addiction. Research consistently shows that peer support in group settings improves treatment engagement and reduces relapse risk. Participants log in around 5 or 6 p.m. after work, and licensed clinicians guide structured skill-building while the group processes their week together.
One-on-One Sessions Address Individual Recovery Goals
Individual therapy happens separately from group work, usually weekly, allowing your clinician to address your specific triggers, co-occurring mental health conditions, and personalized recovery goals without the group dynamic. These sessions occur either the same evening as group therapy or on another scheduled night, depending on your treatment plan. Your clinician tracks your progress through measurement-based care and adjusts your treatment approach based on how you respond. This personalized attention ensures that the program addresses your unique circumstances rather than applying a one-size-fits-all framework.
Remote Testing Creates Accountability Without Barriers
Remote drug and alcohol testing provides the accountability structure that keeps recovery on track. Participants complete tests from home using standardized protocols, eliminating transportation or scheduling conflicts that prevent participation in traditional programs. Testing happens on a schedule your clinician establishes based on your substance use history and risk factors. This testing framework isn’t punitive; it’s protective, giving you objective data about your progress and creating measurable markers of stability that matter when you’re rebuilding trust with family and employers.
Medication Management Supports Physical and Mental Health
Medication management services are available when needed, with psychiatrists or nurse practitioners monitoring prescriptions and supporting withdrawal management or co-occurring conditions. The clinical team holds you accountable, tracks your progress, and adjusts your treatment plan based on your response. This entire structure delivers what traditional daytime programs cannot: treatment that acknowledges your real life as a working professional with family obligations. You’re not abandoning work responsibilities, explaining absences to supervisors, or scrambling for childcare coverage. The rigor remains intact because the clinical framework still maintains accountability while fitting around your actual schedule.
What Makes Evening Structure Work for Busy Lives
The practical flow assumes you’re a functional adult with work commitments and family obligations, not someone whose life stops during treatment. Your clinician establishes testing frequency based on your individual risk profile, and the clinical team adjusts your treatment plan as you progress. This model works because it removes the friction that prevents people from starting treatment in the first place, yet maintains the same clinical intensity and structure that drives real recovery. When your program fits your life instead of forcing your life to stop, you attend consistently, engage more deeply, and build sustainable momentum toward lasting change. Understanding this structure is one thing; knowing how to actually access it is another.
What Actually Changes When Treatment Fits Your Schedule
The Logistics That Stop People From Starting
The barrier isn’t motivation or commitment to recovery. It’s logistics. A person working full-time cannot attend a daytime IOP without sacrificing income, risking employment, or inventing explanations to supervisors. Daytime programs require 9–15 hours weekly during standard business hours, which translates to taking extended time off or maintaining a lie about where you are. For a parent, the logistics multiply: arranging childcare for three to five afternoons per week costs money you don’t have while in treatment, or forces you to pull kids from school early. Transportation adds another layer of complexity. Someone without reliable access to a car cannot attend daytime sessions across town, especially if they’re managing withdrawal symptoms or mental health crises that make driving unsafe. These aren’t minor inconveniences. They’re deal-breakers that keep people from starting treatment at all.
How Evening Timing Removes Friction
Evening IOP eliminates these barriers entirely by delivering structured clinical care after 5 p.m., when your workday ends and childcare logistics simplify. You attend sessions from home through telehealth, removing the transportation problem altogether. Your paycheck stays intact because you’re not missing work. Your kids stay in school because treatment happens after they’re home.

The clinical intensity doesn’t change-you still receive individual therapy, group sessions with licensed clinicians, and remote drug and alcohol testing-but the timing removes the friction that makes treatment impossible for working people.
Employment Retention Proves the Model Works
Programs reporting outcomes from evening models consistently show that participants maintain employment during treatment, compared to significantly lower employment retention in daytime programs. When someone can attend treatment without sacrificing their job, their financial stability, or their parenting responsibilities, they show up consistently. Consistent attendance drives better outcomes because recovery requires sustained engagement, not sporadic participation squeezed around life obligations.
Telehealth Solves Transportation and Access Problems
Telehealth specifically eliminates transportation barriers that affect rural clients, people without reliable vehicles, and those managing disabilities that make commuting difficult. Testing remotely means you complete accountability measures from home using standardized protocols, removing the transportation conflict that causes people to miss testing appointments in traditional programs. This practical accessibility matters because treatment completion depends on showing up. When your program fits your actual life instead of demanding your life stop, you stay engaged long enough for clinical interventions to work. That’s not a minor advantage. That’s the difference between treatment that remains theoretical and treatment that actually happens.
Final Thoughts
The biggest obstacle to addiction treatment isn’t willingness or commitment. It’s the demand that you stop your life to fix your life. Traditional daytime programs force working professionals into an impossible position: sacrifice your paycheck, risk your job, or skip treatment entirely. Evening IOP accessibility changes that equation completely by delivering clinical care after 5 p.m., when you can actually participate without sacrificing your career or family responsibilities.
When treatment happens in the evening, you keep your job, maintain your income, and stay present for your family while the clinical intensity remains unchanged. You receive individual therapy with licensed clinicians, participate in evidence-based group sessions, and complete remote drug and alcohol testing that creates real accountability. Programs using evening models consistently report that participants maintain employment during treatment, compared to significantly lower employment retention in daytime programs-that’s the foundation of long-term stability.
We at EveningIOP have built a program specifically for this reality, with live telehealth group therapy, one-on-one sessions, and remote testing all happening in the evening to remove the transportation barriers and scheduling conflicts that derail people from traditional programs. You pursue recovery without disrupting work or home responsibilities, and accessible care leads to better outcomes because it acknowledges how real people actually live.


