Addiction doesn’t care about your reputation or your schedule. The fear of being discovered keeps millions from getting help they desperately need.
At EveningIOP, we built our program around confidential addiction care because privacy shouldn’t be a luxury-it should be standard. When treatment happens on your terms, in your space, recovery becomes possible.
Why Confidentiality Matters in Addiction Treatment
Stigma stops people from seeking help far more effectively than addiction itself. Research from the Substance Abuse and Mental Health Services Administration shows that fear of judgment, legal consequences, and workplace discovery prevents millions from entering treatment. When someone considers calling a treatment center, the first thought isn’t clinical-it’s practical. Will my employer find out? Will this show up on a background check? Will my family be told? These aren’t paranoid concerns. They’re legitimate barriers rooted in real consequences. Federal law protects addiction treatment records under 42 C.F.R. Part 2, meaning your treatment information cannot be disclosed without your written consent, with limited exceptions for medical emergencies or mandatory reporting situations like child abuse. This protection exists specifically because privacy in substance use disorder treatment directly impacts whether people seek care at all. Studies consistently show that patients who trust their privacy disclose their full history more openly, comply with treatment more reliably, and stay engaged long enough for recovery to take hold.
Visibility Creates Real Barriers
Traditional in-person programs create visibility problems that telehealth eliminates. Driving to a clinic during evenings or weekends, sitting in a waiting room, or being seen entering a facility introduces risk. Colleagues notice patterns. Family members ask questions. Neighbors recognize the building. This isn’t theoretical-it’s why many people delay treatment for years or never seek it at all. Evening programs delivered through secure telehealth platforms remove these friction points entirely. You attend sessions from home or a private location, using the same video technology millions use for work calls. No one knows what you’re doing unless you tell them. The American Psychiatric Association documents that treatment engagement increases significantly when patients control who knows about their care.

Sessions happen through HIPAA-compliant platforms where licensed clinicians deliver intensive outpatient care without the visibility of traditional brick-and-mortar facilities. Your treatment stays between you and your care team.
Privacy Strengthens Clinical Outcomes
People in confidential care disclose more honestly and stay longer in treatment. The Institute of Medicine found that comprehensive, integrated treatment addressing medical, psychiatric, social, and vocational needs produces better outcomes-but only if patients actually show up and engage fully. Confidentiality removes the barrier that prevents honest participation. Someone struggling with relapse urges talks more openly with a clinician they trust to keep that information private. Someone managing co-occurring depression or anxiety can address it without fearing that mental health treatment will be discovered alongside addiction care. This isn’t just about comfort. It’s about clinical effectiveness. Patients who feel secure in their privacy follow treatment plans more consistently, attend sessions more reliably, and remain engaged during the critical early months when relapse risk is highest.

The question isn’t whether confidentiality matters-it clearly does. The real question is how to access treatment that actually protects your privacy while delivering the clinical intensity your recovery requires.
How Evening IOP Protects Your Privacy
The technical infrastructure matters less than what it actually accomplishes: your treatment stays confidential, your sessions don’t appear on household internet histories that family members might see, and no one at work notices a pattern of absences. Evening IOP uses HIPAA-compliant telehealth technology, which means sessions encrypt end-to-end and records store on secure servers that meet federal standards. More importantly, you log in from wherever you choose-home, a parked car, a coffee shop, anywhere with internet. There’s no waiting room where a coworker might spot you, no clinic sign visible from a parking lot, no paper trail of bills arriving at your house.
Secure Technology Built for Privacy
The platform Evening IOP uses handles confidential work calls for Fortune 500 companies, which means the infrastructure was built for privacy from the ground up. Your sessions transmit through encrypted channels. Your records stay locked behind security protocols that federal regulators require. The system doesn’t create visible patterns-no repeated trips to a physical location, no scheduling conflicts that demand explanation, no evidence that you’re in treatment unless you choose to share that information.
Federal Law Protects Your Records
Licensed clinicians at Evening IOP are bound by the same confidentiality standards that protect any healthcare provider, reinforced by 42 C.F.R. Part 2, which specifically governs substance use disorder records. Your treatment information cannot leave our care team without your written consent, period. No employer can demand access. No insurance company can share details with anyone else. No family member can call and learn what you discussed in sessions.
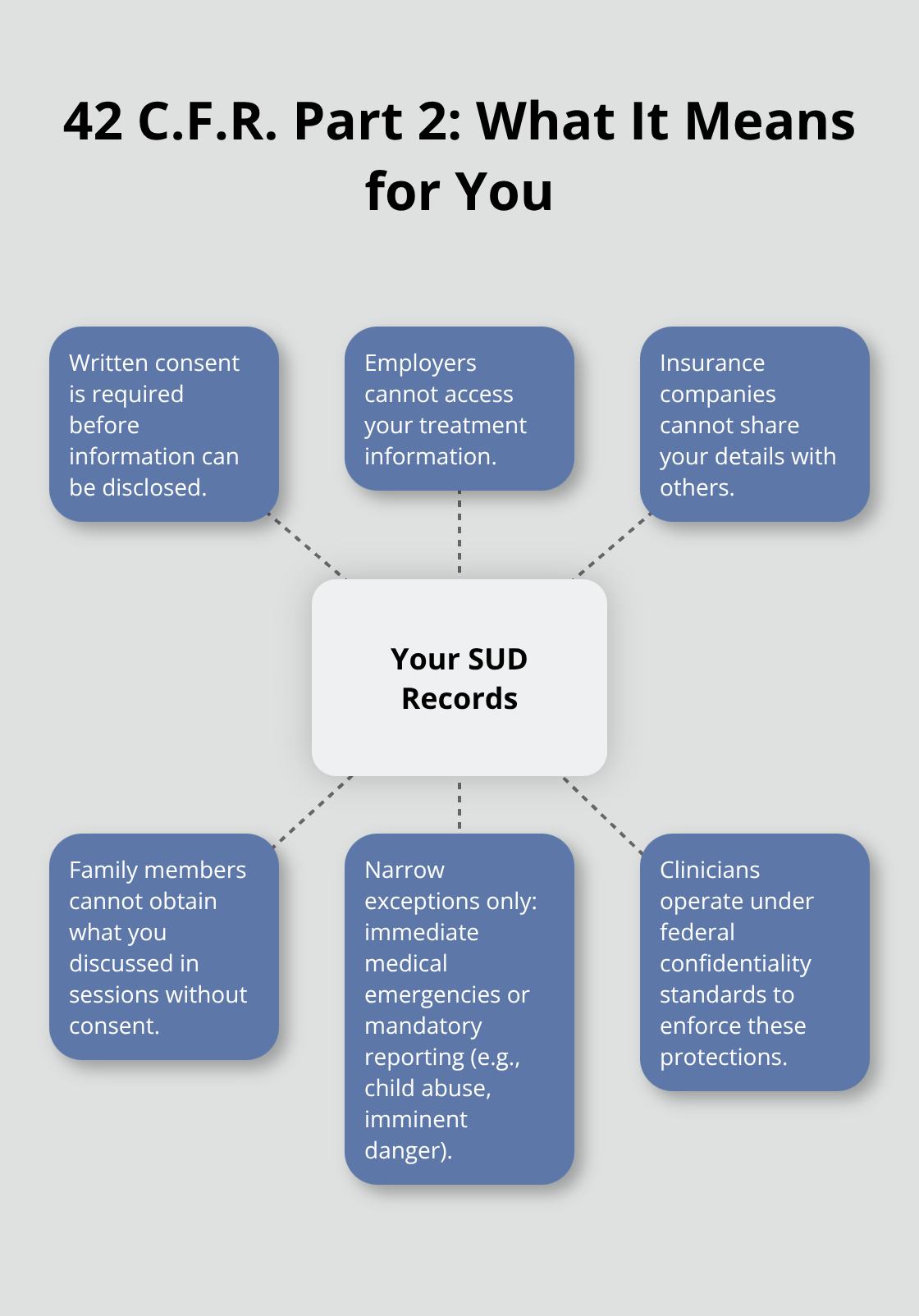
The only exceptions are narrow and legally defined: immediate medical emergencies or mandatory reporting for child abuse or imminent danger. Everything else requires your explicit permission first.
Evening Sessions Remove Workplace Barriers
What separates effective confidential care from merely private care is whether you actually trust it enough to be honest. Evening IOP structures sessions so you can attend without disrupting work, which removes the most obvious barrier to consistent attendance. You don’t take time off that raises questions. You don’t reschedule meetings or explain absences. You log in after work or on weekends when your schedule already allows flexibility. This matters clinically because people who attend sessions consistently-who don’t have to choose between treatment and their job-show better outcomes.
Clinicians Who Understand Confidential Recovery
Licensed clinicians who specialize in substance use disorders understand that recovery happens fastest when you can be completely honest about what you’re experiencing. That honesty only happens if you genuinely believe nothing you say will follow you back into your workplace or family life. Federal law protects that, but the real protection is the structure: evening programs, telehealth format, clinicians trained to handle sensitive disclosures, and systems designed so your treatment simply doesn’t intersect with the parts of your life you’re trying to protect.
The infrastructure protects your privacy. The structure protects your engagement. Together, they create the conditions where honest conversation becomes possible-and honest conversation is where real recovery begins.
Taking the First Step Toward Recovery
Your first session at an evening intensive outpatient program differs from traditional addiction treatment. You won’t sit in a waiting room or complete forms by hand. You’ll log in from home during evening hours, connect with a licensed clinician via secure video, and start building a recovery plan tailored to your specific situation. The intake process typically takes 60 to 90 minutes and covers your substance use history, any co-occurring mental health conditions, medical background, social supports, and what recovery looks like for you personally. This matters because effective treatment addresses the whole person-not just the addiction itself.
What to Expect During Intake
If you have depression, anxiety, trauma, or other conditions alongside substance use, those conditions get identified and addressed simultaneously. Prepare for your first session by being honest about everything: your drug or alcohol use, how long it’s been happening, what you’ve tried before, what triggers your use, and what barriers have stopped you from seeking help. Clinicians aren’t there to judge. They’ve heard it before, and they need the full picture to recommend the right level of care and treatment approach. Write down any medications you take, any allergies, and any previous treatment you’ve received. Have your insurance information ready if you have it, though lack of insurance doesn’t prevent you from accessing care through community health centers or sliding-scale programs.
Why Evening Programs Increase Attendance
What happens after intake determines whether you stay engaged or drop out. Comprehensive treatment combining medical, psychiatric, social, and vocational support produces the best outcomes, but only if you actually show up. Evening programs remove the most common excuse: you can’t attend because work conflicts with daytime sessions. You can’t explain absences to your boss. You can’t take time off without raising questions. Evening IOP structures treatment around your actual life, which means you’re far more likely to attend consistently.
Building Trust With Your Treatment Team
Trust with your treatment team develops through honesty and consistency. Your clinician needs to know when you’re struggling, when you’re having cravings, when you’re thinking about using again, when something in your life is falling apart. That honesty only happens if you genuinely believe what you say stays confidential and won’t be used against you. Federal law protects your records, but trust comes from consistent experience with clinicians who listen without judgment and follow through on what they say. Come to sessions on time. Complete the work assigned between sessions. Adjust your treatment plan if what you’re doing isn’t working. Recovery isn’t passive. It requires active participation, and the clinicians who specialize in substance use disorders understand that the people who recover are the ones who show up, speak up, and stay engaged even when it’s hard.
Final Thoughts
Confidentiality forms the foundation that makes addiction treatment possible. Without privacy protections, millions stay silent about their struggle, delay seeking help for years, and suffer alone rather than risk exposure. Federal law recognizes this reality through 42 C.F.R. Part 2, which shields substance use disorder records from disclosure without consent. What transforms law into actual recovery is a treatment structure that removes the practical barriers keeping people away-evening sessions that fit your life, secure telehealth platforms that eliminate waiting rooms, and licensed clinicians who understand that honest conversation only happens when you genuinely trust your privacy.
People who access confidential addiction care disclose more honestly, attend sessions more consistently, and stay engaged through the critical early months when relapse risk peaks. This matters clinically because when you can speak openly about cravings, triggers, co-occurring mental health conditions, and what’s actually happening in your life, clinicians can help you address the real problems driving your substance use. The structure itself protects your privacy-no facility signs, no patterns coworkers notice, no evidence that you’re in treatment unless you choose to share that information.
Your path forward starts with a confidential conversation. EveningIOP provides evening care designed for people who need treatment without disrupting work or family. Reach out and be honest about what you’re struggling with.


