Recovery doesn’t stop when the workday ends. At EveningIOP, we know that fitting treatment into a busy schedule is one of the biggest barriers people face when seeking help.
Telehealth relapse prevention evenings remove that barrier by bringing professional support directly to you at times that actually work. This guide walks you through how evening programs work, why they’re effective, and how to find the right fit for your recovery.
What Happens During a Telehealth Relapse Prevention Evening
Telehealth relapse prevention evenings operate as structured, real-time sessions where licensed clinicians monitor your progress and respond to emerging challenges before they escalate. EveningIOP combines three core components that work together to prevent relapse: remote drug and alcohol testing that provides objective accountability, one-on-one sessions with licensed clinicians who adjust your treatment plan based on test results and your reported stress levels, and interactive group therapy where you connect with peers facing similar struggles. The HEALing Communities Study, led by NIDA in partnership with SAMHSA, found that telehealth for opioid use disorder increased treatment retention compared to standard care, showing that remote monitoring actually works. During your session, a clinician reviews your week, identifies high-risk moments, and teaches specific coping techniques you can use immediately when cravings hit. Group sessions aren’t passive lectures; they’re peer-led discussions where participants share what triggered their urges and what strategies helped them stay grounded.
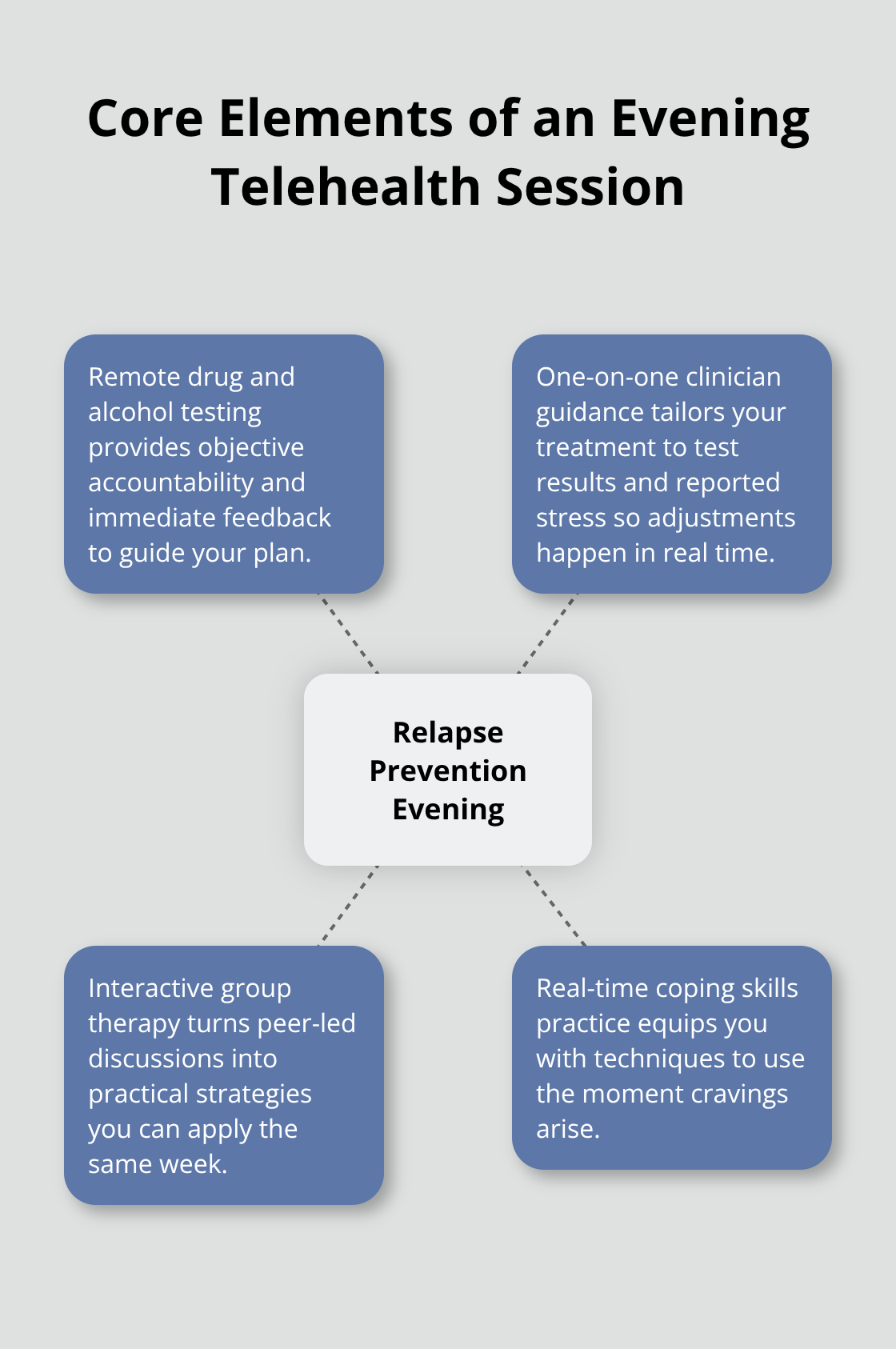
Research shows that greater mutual-help group attendance is linked to lower addiction-related symptoms, meaning the peer connection itself becomes a relapse-prevention tool.
Real-Time Accountability Through Remote Testing
Remote drug and alcohol testing removes the guesswork from recovery. When you test clean, it reinforces your commitment and gives you concrete proof of progress to discuss with your clinician. When results show substance use, your clinician doesn’t shame you; they use that information to identify what happened that week and adjust your coping strategies. This creates a feedback loop where testing data directly informs your treatment adjustments rather than waiting weeks between appointments. Studies show that structured post-treatment plans with regular check-ins are associated with lower rates of heavy drinking and longer abstinence, and testing serves as the objective foundation for those check-ins.
Clinician Guidance Tailored to Your Triggers
Licensed clinicians during evening sessions focus on your specific relapse patterns, not generic advice. They help you map which situations, emotions, or people consistently put you at risk, then build coping techniques matched to those exact triggers. If stress at work drives your cravings, your clinician teaches stress-management tools you can deploy during your workday. If evening isolation is your weak point, they help you structure your evenings differently. This one-on-one time also allows medication adjustments if you’re on medication-assisted therapy, since a multidisciplinary team can tailor your regimen as your needs evolve throughout your recovery.
Peer Connection as a Relapse-Prevention Tool
The group component transforms recovery from an isolated struggle into a shared experience. Peers in your evening sessions face the same work pressures, family obligations, and cravings you do-they understand your reality in ways a clinician alone cannot. When someone shares how they handled a difficult moment at work or managed weekend stress, you gain practical strategies you can adapt to your own life. This peer accountability (combined with clinician oversight) creates multiple layers of support that catch warning signs early and prevent small slips from becoming full relapses.
Why Evening Programs Actually Work for Working Adults
The reality is blunt: daytime treatment schedules don’t fit most people’s lives. If you work a traditional 9-to-5 job, attending a daytime appointment means taking time off, risking your employer noticing, and potentially jeopardizing your income or health insurance coverage. Evening telehealth relapse prevention solves this by delivering intensive care after work ends, which means you stay employed, keep your paycheck, and maintain the stability that supports recovery. You attend from home or any private location, eliminating commute time and the anxiety of sitting in a waiting room where you might run into a coworker. Research shows that improving employment status leads to better long-term recovery outcomes for people in treatment.
Evening Sessions Fit Your Real Schedule
Evening programs operate between 5 and 8 p.m., the window when most working professionals are available but treatment centers typically close their doors. You’re not juggling sick days or making excuses to your boss; you log in at 6 p.m. and your session happens. That consistency matters because structured post-treatment plans with regular check-ins support sustained recovery. Studies tracking online mutual-help groups and remote treatment programs show that when people can attend without sacrificing work or family time, they actually show up consistently.

Adherence across telehealth programs varies depending on the substance and program design, but the highest adherence appears when scheduling removes barriers.
Family Life Stays Intact
Evening programs also mean you’re not choosing between recovery and your family. Parents can be present for dinner, homework help, and bedtime routines instead of missing those moments for a 2 p.m. appointment. For older adults managing multiple daytime medical appointments or transportation challenges, evening sessions remove a major logistical barrier entirely. The scheduling flexibility doesn’t compromise care intensity either-evening IOPs deliver the same clinical rigor as daytime programs, with group therapy, individual sessions, and monitoring compressed into focused evening hours.
Real-Time Response to Your Triggers
Evening programs let you address relapse triggers in real time. If your high-risk moments happen after 5 p.m. (stress unwinding from work, isolation at night, boredom after family responsibilities end), your clinician can teach coping techniques you practice immediately that same evening rather than waiting until your next appointment days later. Telehealth means you’re not limited to whatever clinician happens to be available at your local center; you access licensed professionals regardless of geography. Many insurance plans cover evening telehealth sessions at the same rate as daytime appointments, making cost predictable and removing another barrier to consistent attendance.
The next step is understanding what actually triggers your relapse risk and how to build defenses against those specific moments.
Common Relapse Triggers and Prevention Strategies
Most people think relapse happens randomly, but it doesn’t. Research tracking substance use patterns shows that specific situations, emotional states, and environmental cues consistently precede relapse. Your job is to identify which ones apply to your life, then build defenses before those moments arrive.
Work Stress as a High-Risk Trigger
Work stress ranks as one of the highest relapse triggers for employed adults. Workplace pressure, conflicts with supervisors, and job insecurity directly correlate with increased cravings and relapse risk. Evening programs matter here because they let you address work-related stress the same day it happens rather than sitting with it all night. If Mondays after difficult meetings trigger cravings, your clinician can teach you a specific technique you practice that evening.
Evening Isolation and Unstructured Time
Evening isolation also drives relapse more than people admit. The hours between 6 p.m. and midnight account for a disproportionate share of relapse episodes, particularly for people living alone or with unsupportive family members. Boredom, loneliness, and the absence of structure during evening hours create vulnerability. Evening telehealth relapse prevention directly counteracts this by providing peer connection and clinician support during your actual high-risk window.
Family Conflict and Unexpected Triggers
Family conflict ranks equally high as a relapse driver. Arguments with a partner, tension around household responsibilities, or conflict with adult children can trigger cravings within minutes. Identifying these patterns means you know which conversations are dangerous for your recovery and which people or situations require extra coping preparation. Some people relapse during positive events too-celebrations, social gatherings, or moments when stress temporarily lifts can catch people off guard because they expect relapse only during crisis. Your clinician helps you prepare coping responses for these situations so they don’t become excuses to use.

Building Concrete Responses to Your Specific Triggers
Knowing your triggers means nothing without a practiced response ready to deploy. Effective coping techniques aren’t generic relaxation advice. They’re specific actions matched to your exact trigger and situation. If work stress drives your cravings, stress-management techniques matter less than a concrete plan like a 10-minute walk, a call to your sponsor, or journaling about what happened before you return home. If evening isolation is your vulnerability, your response isn’t positive thinking; it’s committing to a specific activity during that window, whether that’s attending an online mutual-help group, calling a peer from your evening sessions, or structured exercise.
Research shows that people with written relapse-prevention plans that include specific coping responses for identified triggers have substantially lower relapse rates than those with general awareness alone. During evening sessions, your clinician works with you to map your specific triggers, then practices responses until they become automatic. This rehearsal matters. When cravings hit, your brain doesn’t have time to think through options; it needs an ingrained response ready to execute. Your group peers also become a coping tool. When someone in your evening session describes handling a trigger successfully, you gain a tested strategy you can adapt. This peer learning accelerates your own coping development because you’re learning from people navigating identical challenges in real time, not from a therapist’s textbook.
Final Thoughts
Evening telehealth relapse prevention evenings work because they meet you where you actually are: working, managing family responsibilities, and vulnerable during the hours when most treatment centers close. Structured evening programs with real-time monitoring, peer support, and clinician guidance reduce relapse rates and keep people engaged in recovery longer than sporadic appointments ever could. Your triggers won’t disappear, but with practiced coping responses matched to your specific high-risk moments, you gain the tools to move through them without using.
We at EveningIOP built live telehealth evening Intensive Outpatient Programs that combine interactive group therapy, one-on-one sessions with licensed clinicians, and remote drug and alcohol testing-all designed so you attend from home after work ends, maintain your employment and income, and access DHCS-licensed, Joint Commission-accredited care without disrupting your family or your paycheck. Contact a program that offers evening telehealth relapse prevention and ask specific questions: How many sessions per week? What’s the clinician-to-participant ratio? Do they offer medication-assisted therapy if you need it? Will your insurance cover evening sessions?
Recovery is possible, and thousands of working professionals and parents have rebuilt their lives through evening programs that respect their reality instead of forcing them to choose between treatment and everything else. Your recovery doesn’t have to wait until you can afford to take time off work or until your family situation changes-it can start this week, in the evening, from your home.