Substance use disorder treatment through telehealth offers real flexibility and accessibility, but navigating insurance coverage can feel overwhelming. At EveningIOP, we’ve helped countless people understand how insured telehealth SUD treatment actually works in practice.
This guide walks you through your insurance benefits, finding providers who accept your plan, and what to expect from treatment. You’ll have the clarity you need to start your recovery with confidence.
How Your Insurance Actually Covers Telehealth SUD Treatment
Your insurance plan’s coverage for substance use disorder treatment depends on three things: your specific policy, your insurer’s network, and what you’re willing to pay out of pocket. Most commercial insurance plans, Medicare Advantage, and Medicaid cover telehealth SUD treatment, but the details matter enormously.
Call Your Insurer and Ask the Right Questions
Contact the member services number on the back of your insurance card and ask directly whether your plan covers telehealth behavioral health services and SUD-specific treatment. Request the plan document section on mental health and substance use benefits-this tells you your deductible, copay amounts, and whether prior authorization is required. Many insurers’ reimbursement policies for telehealth have changed, particularly for Medicare beneficiaries receiving care in their homes.
According to research from JAMA Network Open published in 2025, telehealth SUD treatment services grew from 44.6 to 10,974.3 services per month between 2019 and 2023 among insured adults, and commercially insured individuals saw a 1% increase in overall treatment utilization during this period. This expansion happened because insurers recognized that telehealth reduces no-shows and increases access without sacrificing outcomes.
Understand In-Network vs. Out-of-Network Costs
When you call your insurer, also ask whether they have a preferred provider list for SUD treatment. In-network providers mean lower out-of-pocket costs for you. Out-of-network providers typically cost 30% to 50% more, though some plans offer out-of-network benefits if you meet specific criteria like no in-network options within a certain distance.
After insurance pays its share, you’ll owe your deductible, copay per session, or coinsurance (a percentage of the total cost). If your plan requires prior authorization, your provider handles this-it’s not your responsibility-but you should confirm this happens before your first session to avoid unexpected bills later.

Get Your Out-of-Pocket Estimate in Writing
Request an estimate from your insurance company that shows what they’ll pay and what you’ll owe per session. This estimate is free and takes minutes but saves you from billing surprises. Ask whether your plan covers medication-assisted treatment options if that’s part of your plan-coverage varies by insurer and plan type.
If costs are still prohibitive, ask your provider about sliding scale fees or payment plans; many treatment programs offer these options regardless of insurance. Call your insurer directly to confirm coverage details, and SAMHSA’s National Helpline at 1-800-662-HELP can also help you understand coverage questions and connect you with providers who work with your specific insurance type.
Once you understand your coverage and costs, the next step is finding a telehealth SUD treatment program that actually accepts your insurance and meets your clinical needs.
Finding Telehealth SUD Programs That Accept Your Insurance
Start With Official Treatment Locators
FindTreatment.gov, SAMHSA’s official locator, filters by insurance type, location, and treatment modality. When you search, select telehealth and your specific insurance plan to see only programs accepting your coverage. This eliminates the back-and-forth of calling programs that don’t accept Medicaid, Medicare Advantage, or your commercial plan. For opioid-specific treatment, the Opioid Treatment Program Directory lists accredited programs by state, though many also offer telehealth beyond opioid treatment.
Verify Credentials and Accreditation Before You Call
Before contacting any program, verify it holds a state license and accreditation from Joint Commission or CARF. These credentials signal clinical quality and insurance compliance. When you call, ask directly whether the program holds current accreditation, whether it’s DHCS-licensed or equivalent in your state, and whether it’s LegitScript-certified. This certification matters because it shows the program meets rigorous telehealth standards and handles controlled substance prescriptions responsibly.
Navigate Prior Authorization Requirements
Prior authorization is where most people stumble. Ask the program whether they handle prior authorization submission or whether you do-ideally, the program submits it for you before your first session. Some programs submit authorization requests the same day you enroll; others wait until intake. If your plan requires authorization and the program hasn’t submitted it before your start date, call your insurer directly and provide your authorization request number to track progress.
Insurers deny requests if the program isn’t in-network, if your diagnosis doesn’t meet medical necessity criteria, or if the requested duration exceeds what your plan allows. Ask your program upfront what happens if authorization is denied. Reputable programs won’t charge you if they failed to obtain it.
Get Written Insurance Confirmation
Confirmation of insurance acceptance before starting is non-negotiable. Have the program send you a written confirmation showing your plan name, member ID, what they’ll bill, and your estimated copay or coinsurance per session. This confirmation protects you if billing disputes arise later.

Programs that handle these details systematically-like those offering evening schedules-recognize that patients often work during business hours and can’t manage insurance logistics themselves.
With your insurance verified and a program selected, you’re ready to understand what actually happens during your first telehealth sessions and how treatment unfolds week to week.
What Happens During Your First Telehealth Sessions
Your first telehealth SUD treatment session isn’t therapy yet-it’s clinical assessment and intake. The clinician asks detailed questions about your substance use history, medical conditions, medications, psychiatric symptoms, and what prompted you to seek treatment now. They use standardized screening tools like the PHQ-9 for depression and GAD-7 for anxiety to measure baseline mental health. This assessment determines your treatment intensity level, whether medication-assisted treatment fits your situation, and what modalities make sense for your recovery. Expect this first session to last 60 to 90 minutes and feel thorough-clinicians need this information to build an accurate treatment plan. You’ll also discuss confidentiality rules, what happens if you miss sessions, and how the program handles crises or emergencies. Many programs ask you to confirm your home internet reliability and device setup during intake because telehealth only works if your connection is stable. Some programs send you a test link before your first appointment so you can troubleshoot audio or video issues beforehand.
Your Weekly Schedule and Session Structure
Insured telehealth SUD treatment typically involves individual counseling sessions, group therapy sessions, and regular clinical monitoring over 9 to 12 weeks of intensive outpatient care. Research from a study of 3,642 adults discharged from intensive outpatient programs showed participants averaged 9.2 individual counseling visits and 6.3 group therapy visits during their first 90 days, with about 78 percent using individual telehealth and 34 percent using group telehealth.
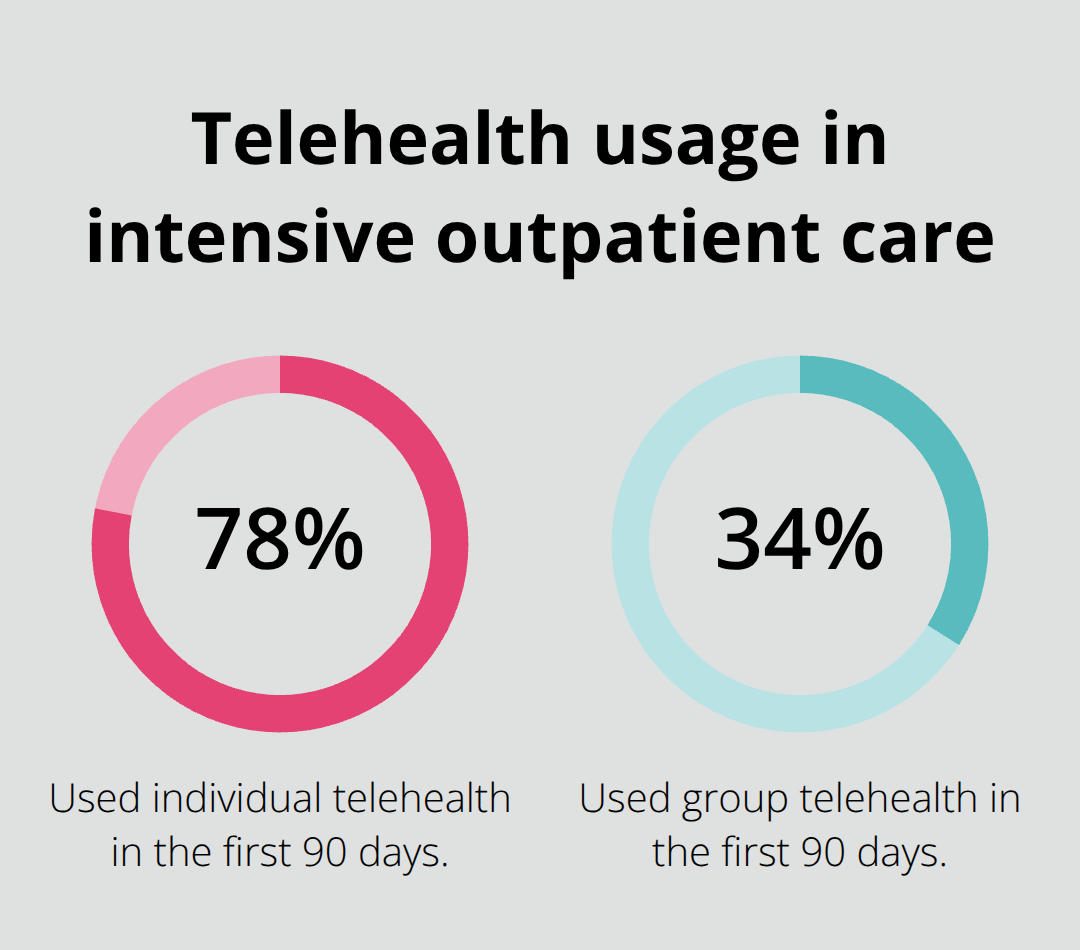
Your insurance covers these sessions at the copay rate you confirmed before starting. Group sessions usually run 90 minutes and include 8 to 15 peers working through evidence-based curriculum on triggers, coping skills, relapse prevention, and recovery maintenance. Individual sessions typically last 50 to 60 minutes and focus on your specific barriers-whether that’s family conflict, work stress, or medication management if you’re on buprenorphine or naltrexone.
Evening and Weekend Availability Matters
Evening and weekend scheduling matters because most people in treatment work or have caregiving responsibilities. Programs offering evening sessions recognize that rigid 9-to-5 hours force people to choose between employment and recovery, and that’s a false choice. Ask your program whether sessions run evenings, weekends, or both before you enroll. Some programs offer both-evening groups at 6 PM or 7 PM and Saturday morning individual sessions-so you can build a schedule that doesn’t force you to miss work or childcare.
Drug Testing and Clinical Monitoring
Insured treatment includes regular drug and alcohol testing because accountability matters for recovery. Your program will specify a testing schedule-typically random urine screens during your first weeks, then less frequently as you progress. Many telehealth programs use remote testing vendors where you visit a local lab or use at-home test kits that you submit digitally. Your clinician reviews results with you at your next individual session, not as punishment but to adjust treatment if needed. If results show substance use, your clinician may recommend increased session frequency, medication-assisted treatment, or peer support meetings rather than discharge. Insurance covers these tests as part of your treatment plan, so ask your program upfront whether testing costs come out of your copay or whether they bill insurance separately. Some programs use fentanyl and xylazine test strips as part of harm reduction-these strips let you check substances for dangerous adulterants before use, and they’re part of evidence-based safety practices that your insurer recognizes as clinically necessary. Your program should also conduct periodic psychiatric assessments-usually at weeks 4 and 8-to monitor depression, anxiety, and cravings using the same standardized scales from your intake. This monitoring prevents you from slipping through the cracks between sessions and gives your clinician real data to adjust your treatment if symptoms worsen.
Final Thoughts
Insured telehealth SUD treatment works when you take three concrete steps: understand your coverage before you start, verify insurance acceptance with your program, and confirm what you’ll owe per session in writing. Most commercial insurance plans, Medicare Advantage, and Medicaid cover telehealth SUD services, but the details vary significantly. Calling your insurer to ask about deductibles, copays, and prior authorization requirements takes 15 minutes and prevents billing surprises later. Research from JAMA Network Open shows that telehealth SUD treatment expanded dramatically between 2019 and 2023, with commercially insured individuals increasing their overall treatment utilization.
Finding a program that accepts your insurance is straightforward if you use official locators like FindTreatment.gov and verify credentials before calling. Ask programs directly whether they handle prior authorization submission, whether they offer evening or weekend sessions that fit your work schedule, and whether they provide written insurance confirmation before your first appointment. Reputable programs make these logistics transparent because they understand that insurance confusion delays treatment entry. What to expect during treatment is predictable: intake assessment, weekly individual and group sessions, regular drug testing, and periodic psychiatric monitoring using standardized tools.
Contact your insurer today using the member services number on your insurance card and request your plan document for mental health and substance use benefits. Then search FindTreatment.gov for telehealth programs accepting your insurance in your area. If you’re looking for a program that combines clinical rigor with evening flexibility, EveningIOP offers live telehealth intensive outpatient care with licensed clinicians, interactive group therapy, and remote drug testing.


