Substance use disorder treatment doesn’t have to fit into a 9-to-5 schedule. At EveningIOP, we’ve built our entire program around the reality that recovery works best when it fits your life, not the other way around.
This 2026 telehealth recovery guide walks you through how evening intensive outpatient programs are changing treatment access for working professionals and parents who need flexibility without sacrificing quality care.
How Telehealth Reshapes Evening Recovery Care
Why Evening Hours Matter for Treatment Access
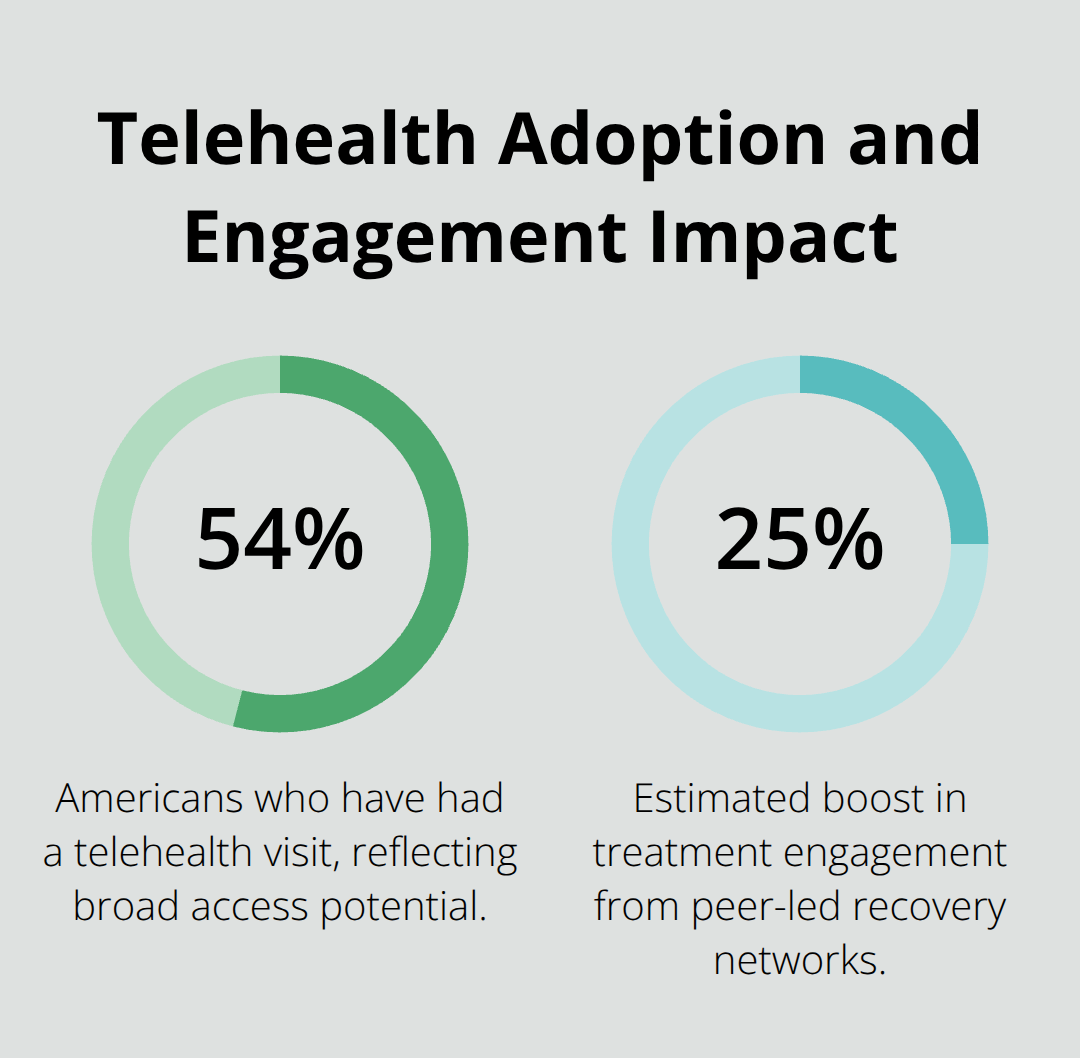
Telehealth didn’t just add evening hours to addiction treatment-it fundamentally changed who can access care and when. The shift matters because 54% of Americans have had a telehealth visit, according to recent data. That statistic alone reveals why traditional 9-to-5 treatment centers miss the people who need them most. Working professionals and parents often cannot take time off for afternoon appointments, and they should not have to choose between their job and their recovery. Evening telehealth programs eliminate that false choice entirely.
Real-Time Clinical Monitoring from Home
The clinical outcomes do not suffer from evening timing. Real-time monitoring through home-based telehealth actually creates tighter oversight than many assume. When you receive treatment from your living room on a video call with a licensed clinician, that clinician observes your environment, sees your physical state, and maintains direct accountability in real time. Remote drug and alcohol testing integrated into evening programs means clinical verification happens on your schedule, not the clinic’s. This continuous monitoring between sessions catches relapse risk early. Structured routines built around evening sessions become sustainable because they fit actual life patterns instead of forcing people into artificial recovery schedules.
Cost Advantages of Evening Telehealth
The financial argument for evening telehealth stands on its own. Inpatient residential treatment costs between $5,000 and $30,000 per month depending on the facility and region. Evening intensive outpatient programs delivered through telehealth typically cost 60-70% less while maintaining clinical rigor. You pay for clinical expertise and peer support delivered efficiently through video, not for facility overhead, meals, or housing. Many programs accept Medicaid and Medicare, and dedicated staff verify your benefits before enrollment so you understand costs upfront. The NIH HEAL Initiative now supports research showing that integrated, personalized care delivered remotely produces comparable outcomes to traditional models-sometimes better, because patients stay in treatment longer when it does not disrupt their lives.
Removing Geographic and Access Barriers
Telehealth removes geographic barriers entirely. Someone in a rural area or underserved community no longer waits months for an appointment with a qualified addiction medicine specialist. They access licensed clinicians immediately through their computer or phone. That accessibility shift matters clinically: earlier intervention reduces severity and improves long-term recovery stability. Evening programs specifically capture the working population that traditional daytime treatment misses entirely, expanding the overall treatment population without sacrificing quality or clinical monitoring intensity.
The next step involves understanding what actually happens inside these evening programs and what you should expect from your first session onward.
Inside an Evening Intensive Outpatient Program
How Evening Programs Structure Your Treatment
Evening intensive outpatient programs operate differently than traditional daytime models, and understanding the actual structure matters because it directly affects your recovery outcomes. Live group therapy sessions bring you face-to-face with peers who face identical challenges, not pre-recorded content or asynchronous modules. These sessions typically run 2-3 hours in the evening and include 8-12 participants with one or two licensed facilitators who guide discussion, challenge avoidance patterns, and hold members accountable to their recovery commitments.
The Power of Peer Support in Evening Groups
Peer support within these groups matters clinically: research shows peer-led recovery networks boost treatment engagement by roughly 25%, and that engagement directly predicts sustained sobriety. You hear from people 30 days sober and people with 18 months clean, which creates realistic expectation-setting and breaks the isolation that drives relapse. This mix of experience levels normalizes the recovery process and shows tangible progress across different timelines.
One-on-One Clinical Work with Licensed Clinicians
One-on-one sessions with licensed clinicians happen separately, usually weekly or twice weekly depending on your treatment plan. These sessions address trauma, co-occurring mental health conditions like anxiety or depression, medication management if you use medication-assisted treatment, and specific relapse triggers unique to your situation. The clinician observes your mood, sleep quality, medication adherence, and environmental stressors, then adjusts your treatment plan based on real clinical data rather than assumptions. Individual sessions stay confidential and allow deeper clinical work that group time cannot provide.
Remote Testing and Accountability
Remote drug and alcohol testing integrates seamlessly into evening programs: you receive testing instructions through a secure patient portal, complete tests at home or a local lab using a network partner, and results reach your clinician within 24-48 hours. This continuous verification removes the temptation to test positive and maintains clinical accountability without requiring you to travel to a facility during work hours. You know testing happens regularly, so craving management becomes active rather than passive.
Why This Structure Works for Working Professionals
The integration of these three components creates accountability without surveillance feeling invasive. Peer group members share specific coping strategies they actually use, not theoretical techniques from a workbook. Licensed clinicians reduce key symptoms to non-problematic levels and improve health and functional status. Evening timing means you attend sessions after work, complete testing on your schedule, and maintain employment or family responsibilities without conflict. That structural fit reduces treatment dropout rates significantly because recovery itself becomes the priority rather than logistics becoming the barrier to staying engaged.
The next step involves knowing exactly what to look for when you evaluate which evening program will support your specific recovery needs and circumstances.
Choosing the Right Evening Telehealth Program for Your Recovery
Verify Accreditation and Licensing Standards
Accreditation status signals whether a program meets measurable safety and clinical standards. The Joint Commission accredits addiction treatment programs that satisfy rigorous criteria for clinical outcomes, staff competency, and patient safety protocols. LegitScript certification adds another verification layer, confirming the program operates legally and maintains compliance with state and federal regulations. Check the program’s website for the Joint Commission accreditation badge and LegitScript certification number-both should appear publicly. If you cannot locate these credentials, contact the program directly and request their accreditation status and last review date. Programs with current accreditation from credible bodies typically renew every three years, so verify the renewal date is recent. State licensing matters equally: addiction treatment programs require DHCS licensing in California or equivalent state licensing in your jurisdiction. You can verify state licenses through your state’s health department website without relying on program marketing claims. This verification step takes 15 minutes and eliminates programs operating without proper oversight.
Assess Program Flexibility and Session Scheduling
Program flexibility determines whether evening care actually fits your life or creates new obstacles. Ask the program specifically about session scheduling: Do evening sessions run at fixed times, or can you attend different sessions each week? Can you attend live group sessions or do they offer recorded alternatives if you occasionally miss a scheduled time? What happens if your work schedule changes or you need to pause treatment temporarily? Programs that offer only rigid 7 PM sessions every Monday, Wednesday, and Friday might not work if your schedule varies. Programs built around evening care typically offer multiple session times throughout the week so you choose which sessions fit your specific schedule, not the other way around. Ask about makeup sessions or asynchronous options for addiction treatment if you travel for work. This flexibility assessment prevents you from enrolling in a program that claims evening availability but forces rigid scheduling that conflicts with your actual responsibilities.
Review Clinical Team Credentials and Experience
Clinical team credentials matter most for your actual treatment outcomes, so request the program’s clinical staff roster with specific credentials: Are group facilitators licensed marriage and family therapists, licensed clinical social workers, or certified addiction counselors? Do individual clinicians hold licensure in addiction medicine, psychiatry, or clinical psychology? What percentage of the clinical team holds credentials beyond basic counselor certification? Programs where the majority of clinicians hold master’s degrees or higher credentials and specialized addiction certifications deliver measurably better outcomes than programs relying primarily on bachelor’s-level staff. Ask about supervisor oversight: who reviews treatment plans, and how frequently? Strong programs conduct monthly clinical reviews and adjust your treatment based on data, not just clinician intuition. Request one reference call with a current patient if possible-programs confident in their outcomes usually allow this. These credential checks eliminate guesswork and ensure you select a program with genuine clinical rigor and qualified clinicians who understand your evening recovery needs.
Final Thoughts
Evening telehealth recovery works because it removes the false choice between treatment and your actual life. The 2026 telehealth recovery guide you’ve just read shows that evening intensive outpatient programs deliver clinical rigor without requiring you to sacrifice employment, family time, or stability. Real-time monitoring, peer accountability, and licensed clinician oversight happen on your schedule, not a facility’s schedule.
Success in night-time care depends on three concrete factors: you need a program with verified accreditation and licensing that proves clinical standards are met, your program must offer genuine scheduling flexibility so evening sessions actually fit your work and family responsibilities, and your clinical team must hold real credentials and experience in addiction treatment. These three factors separate programs that genuinely support recovery from programs that simply offer evening hours. We at EveningIOP provide live, telehealth evening intensive outpatient programs that combine interactive online group therapy, one-on-one sessions with licensed clinicians, and remote drug and alcohol testing-all DHCS-licensed, Joint Commission-accredited, and LegitScript-certified.
Taking the first step means contacting a program and asking specific questions about accreditation, scheduling flexibility, and clinical credentials. You now know what to look for and what questions to ask. Contact EveningIOP and start your recovery journey tonight.


